Cold Hemolysis as the Initial Presentation of B-Cell Acute Lymphoblastic Leukemia: A Case Report
Downloads
Cold hemolysis is a rare but potentially life-threatening condition that may occur as an early manifestation of hematologic malignancies. Prompt recognition is crucial, especially in patients presenting with severe anemia and neurological symptoms, as delayed diagnosis may worsen outcomes.
Methods
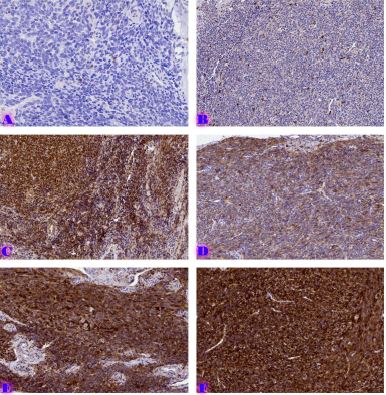
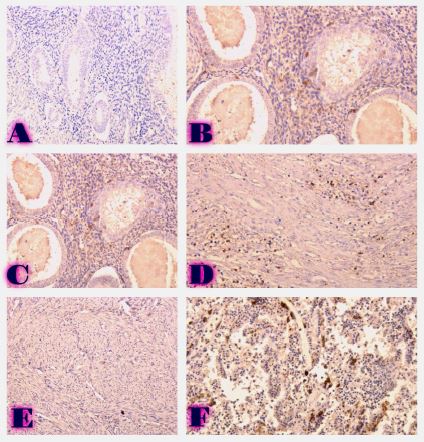
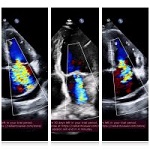
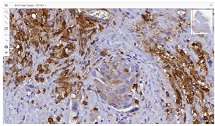
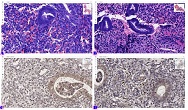
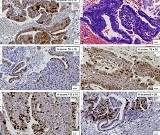
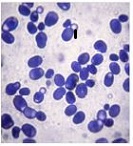
A 39-year-old Lebanese woman was admitted to the emergency department in critical condition with severe generalized weakness, fatigue, marked loss of strength, and anosmia. Laboratory evaluation showed leukocytosis with lymphocytosis and monocytosis, elevated lactate dehydrogenase, and increased indirect bilirubin. Coagulation studies revealed mild hyperfibrinogenemia and hypoprothrombinemia. Abdominal ultrasonography demonstrated no organomegaly or lymphadenopathy but identified a 70-mm hemorrhagic cyst of the right ovary. Peripheral blood smear showed critical pancytopenia with a left shift toward blast cells (~10%). Bone marrow aspiration with cytological and flow cytometric analysis in October 2024 confirmed precursor B-cell acute lymphoblastic leukemia (B-ALL). Hemoglobin was critically low (1.88 g/dL). A bedside temperature-dependent test confirmed cold hemolysis.
Results
The patient was transferred to the intensive care unit and received warmed intravenous fluids and blood component transfusions, resulting in stabilization. She was then transferred to the Onco-Hematology Department. Due to the life-threatening presentation, protocol-based chemotherapy with Hyper-CVAD Part A and B was initiated. She required eight hospitalizations. Hematologic remission was achieved, and at discharge her condition was stable with improved blood counts (hemoglobin 9.96 g/dL). Outpatient therapy was recommended.
Conclusion
Cold hemolysis may represent a rare but severe initial manifestation of precursor B-cell acute lymphoblastic leukemia. Early recognition and prompt intensive management are essential for patient survival and improved prognosis.
Downloads
Berentsen S, Sundic T: Red blood cell destruction in autoimmune hemolytic anemia: Role of complement and potential new targets for therapy. Biomed Res Int. 2015:363278. 10.1155/2015/363278
Swiecicki PL, Hegerova LT, Gertz MA: Cold agglutinin disease. Blood. 2013, 122:1114-1121. 10.1182/blood-2013-02-474437
Barcellini W: New insights in autoimmune hemolytic anemia: From pathogenesis to therapy. Int J Lab Hematol. 2015, 37:14-22. 10.1111/ijlh.12349
Bain BJ: Diagnosis from the blood smear. N Engl J Med. 2005, 353:498-507. 10.1056/NEJMra043442
Berentsen S: How I manage patients with cold agglutinin disease. Br J Haematol. 2018, 181:320-330. 10.1111/bjh.15109
Terwilliger T, Abdul-Hay M: Acute lymphoblastic leukemia: A comprehensive review and 2017 update. Blood Cancer J. 2017, 7:577. 10.1038/bcj.2017.53
Barcellini W, Fattizzo B: Clinical applications of hemolytic markers in autoimmune hemolytic anemia. Dis Markers. 2015:635670. 10.1155/2015/635670
Bain BJ: Blood Cells: A Practical Guide. 2015.
McClure RF, Kaur P, Pagel E: Flow cytometric immunophenotyping in acute leukemia. Clin Lab Med. 2017, 37:753-769. 10.1016/j.cll.2017.07.006
Pui CH, Robison LL, Look AT: Acute lymphoblastic leukaemia. Lancet. 2008, 371:1030-1043. 10.1016/S0140-6736(08)60457-2
Kantarjian H, Thomas D, O’Brien S, et al.: Long-term follow-up of the Hyper-CVAD regimen in adult acute lymphoblastic leukemia. Cancer. 2004, 101:2788-2801. 10.1002/cncr.20668
Arber DA, Orazi A, Hasserjian R, et al.: The 2016 WHO classification of acute leukemias. Blood. 2016, 127:2391-2405. 10.1182/blood-2016-03-643544
Jabbour E, O’Brien S, Ravandi F, Kantarjian H: Monoclonal antibodies in acute lymphoblastic leukemia. Blood. 2015, 125:4010-4016. 10.1182/blood-2014-08-596403
Copyright (c) 2026 Georgian Scientists

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.