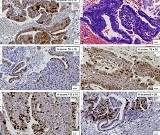
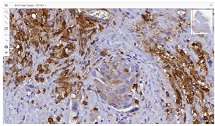
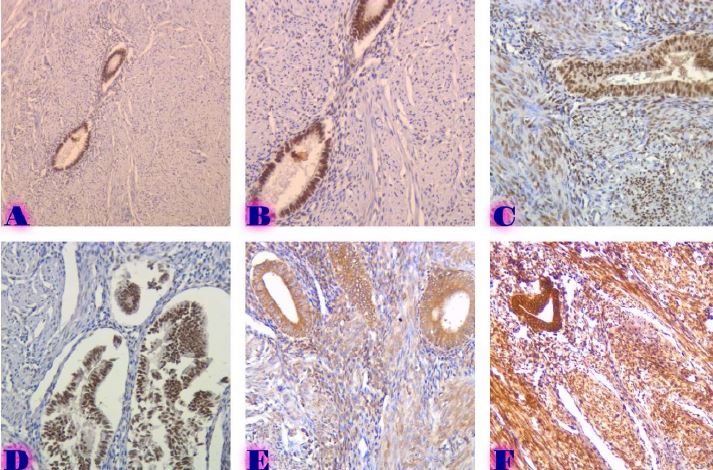
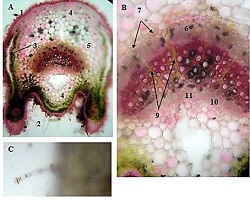
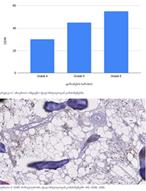
Comparative analysis of features of microenvironment, stem cell and epithelial-mesenchymal transformation of non-invasive papillary bladder carcinoma with invasive carcinoma
Downloads
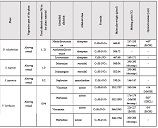
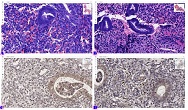
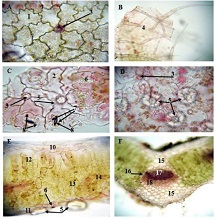
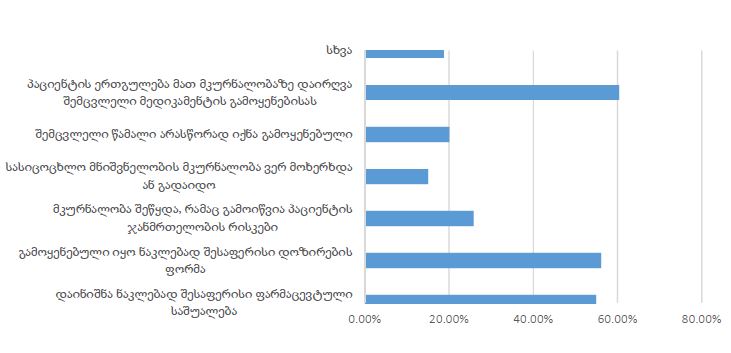
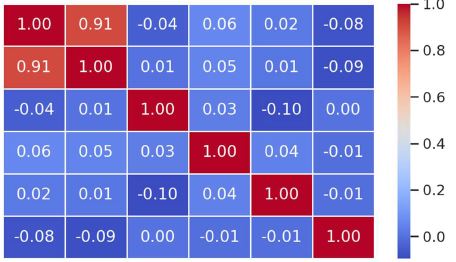
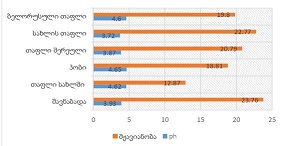
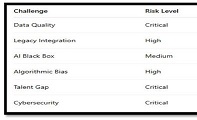
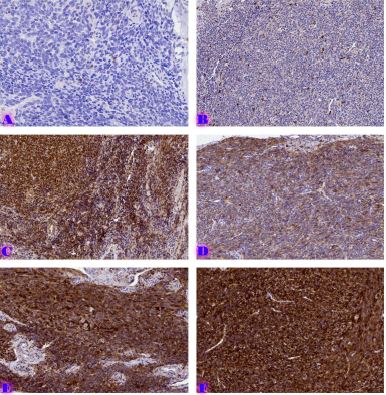
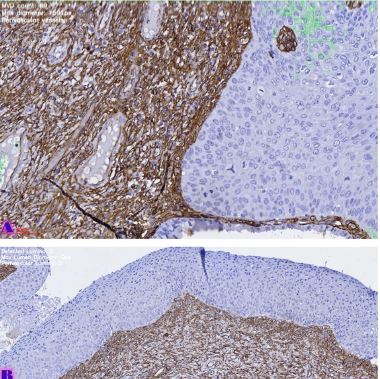
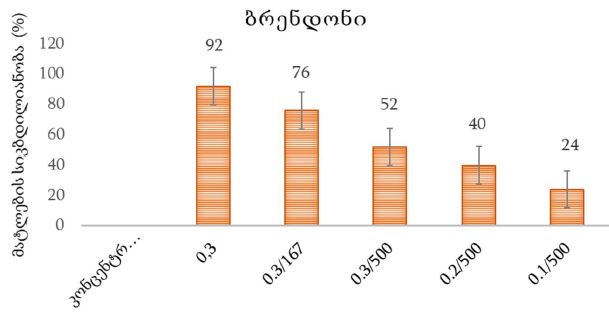
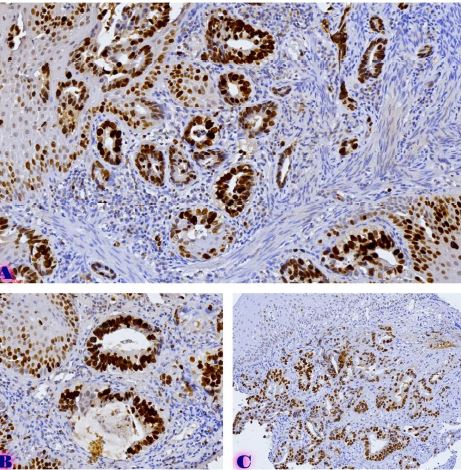
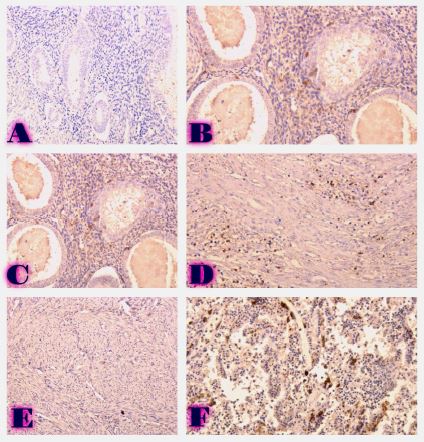
Invasive urothelial carcinoma is the most common bladder malignancy, comprising 90% of all primary bladder carcinomas. According to the statistics of Georgia, according to NCDC data, bladder cancer is the third most common cancer among men. It is more common in men than in women. This pathology takes the 9th place among the most common tumors in the world. Within the framework of our research, a cohort retrograde study was carried out, for which the archival material of the teaching-scientific and diagnostic laboratory of Tbilisi State Medical University for the years 2019-2021 was used. The markers of epithelial-mesenchymal transformation in low- and high-grade non-invasive urothelial carcinomas and invasive urothelial carcinomas, as well as characteristics of the internal tumor microenvironment and stem cell characteristics, were studied. Bladder carcinoma belongs to the heterogeneous group of tumors that have different rates of recurrence, progression and metastasis; It is necessary to develop markers that can be prognostic indicators in bladder tumors, which will greatly improve the clinical management of this type of tumors.
Downloads
D. M. Parkin, “The global burden of urinary bladder cancer.,” Scand J Urol Nephrol Suppl, no. 218, pp. 12–20, 2008, doi: 10.1080/03008880802285032.
E. M. Compérat et al., “Grading of Urothelial Carcinoma and The New ‘World Health Organisation Classification of Tumours of the Urinary System and Male Genital Organs 2016,’” Eur Urol Focus, vol. 5, no. 3, pp. 457–466, May 2019, doi: 10.1016/J.EUF.2018.01.003.
P. A. Humphrey, H. Moch, A. L. Cubilla, T. M. Ulbright, and V. E. Reuter, “The 2016 WHO Classification of Tumours of the Urinary System and Male Genital Organs—Part B: Prostate and Bladder Tumours,” Eur Urol, vol. 70, no. 1, pp. 106–119, 2016, doi: 10.1016/J.EURURO.2016.02.028.
H. Ide, S. Inoue, and H. Miyamoto, “Histopathological and prognostic significance of the expression of sex hormone receptors in bladder cancer: A meta-analysis of immunohistochemical studies,” PLoS One, vol. 12, no. 3, Mar. 2017, doi: 10.1371/JOURNAL.PONE.0174746.
L. Trilla-Fuertes et al., “Biological molecular layer classification of muscle-invasive bladder cancer opens new treatment opportunities,” BMC Cancer, vol. 19, no. 1, Jun. 2019, doi: 10.1186/S12885-019-5858-Z.
A. G. Robertson et al., “Comprehensive Molecular Characterization of Muscle-Invasive Bladder Cancer,” Cell, vol. 171, no. 3, pp. 540-556.e25, Oct. 2017, doi: 10.1016/J.CELL.2017.09.007.
S. J. Yun and W. J. Kim, “Role of the Epithelial-Mesenchymal Transition in Bladder Cancer: From Prognosis to Therapeutic Target,” Korean J Urol, vol. 54, no. 10, p. 645, Oct. 2013, doi: 10.4111/KJU.2013.54.10.645.
A. Yu et al., “Presence of lymphocytic infiltrate cytotoxic T lymphocyte CD3+, CD8+, and immunoscore as prognostic marker in patients after radical cystectomy,” PLoS One, vol. 13, no. 10, Oct. 2018, doi: 10.1371/JOURNAL.PONE.0205746.
H. S. Kim and J. H. Ku, “Prognostic impact of tumor infiltrating lymphocytes in bladder urothelial carcinoma,” Transl Androl Urol, vol. 8, no. Suppl 3, p. S291, 2019, doi: 10.21037/TAU.2019.04.02.
S. F. Faraj et al., “Assessment of tumoral PD-L1 expression and intratumoral CD8+ T cells in urothelial carcinoma,” Urology, vol. 85, no. 3, pp. 703.e1-703.e6, Mar. 2015, doi: 10.1016/J.UROLOGY.2014.10.020.
B. Wang et al., “Programmed death ligand-1 is associated with tumor infiltrating lymphocytes and poorer survival in urothelial cell carcinoma of the bladder,” Cancer Sci, vol. 110, no. 2, pp. 489–498, Feb. 2019, doi: 10.1111/CAS.13887.
T. Horn et al., “The prognostic effect of tumour-infiltrating lymphocytic subpopulations in bladder cancer,” World J Urol, vol. 34, no. 2, pp. 181–187, Feb. 2016, doi: 10.1007/S00345-015-1615-3.
B. Wang et al., “CD103+ Tumor Infiltrating Lymphocytes Predict a Favorable Prognosis in Urothelial Cell Carcinoma of the Bladder,” Journal of Urology, vol. 194, no. 2, pp. 556–562, 2015, doi: 10.1016/J.JURO.2015.02.2941.
H. S. Huang et al., “Prognostic impact of tumor infiltrating lymphocytes on patients with metastatic urothelial carcinoma receiving platinum based chemotherapy,” Sci Rep, vol. 8, no. 1, Dec. 2018, doi: 10.1038/S41598-018-25944-1.
G. Sjödahl et al., “Infiltration of CD3+ and CD68+ cells in bladder cancer is subtype specific and affects the outcome of patients with muscle-invasive tumors,” Urologic Oncology: Seminars and Original Investigations, vol. 32, no. 6, pp. 791–797, 2014, doi: 10.1016/J.UROLONC.2014.02.007.
K. Krpina, E. Babarović, and N. Jonjić, “Correlation of tumor-infiltrating lymphocytes with bladder cancer recurrence in patients with solitary low-grade urothelial carcinoma,” Virchows Archiv, vol. 467, no. 4, pp. 443–448, Oct. 2015, doi: 10.1007/S00428-015-1808-6.

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.