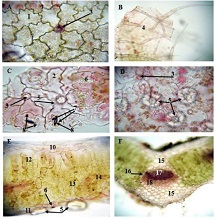
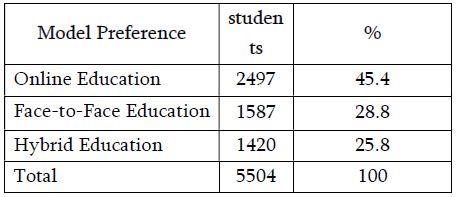
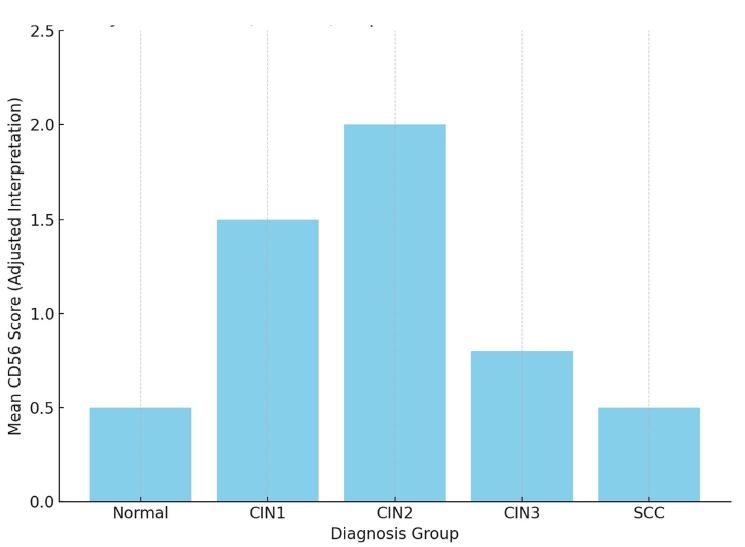
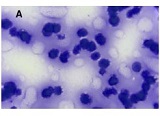
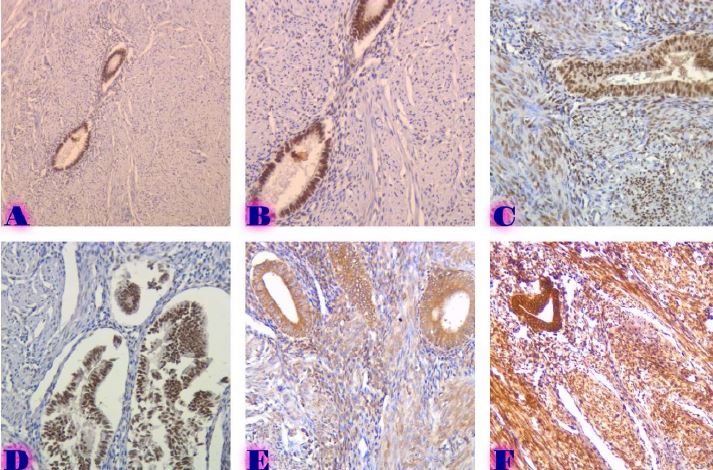
Problematic issues of the mucous membrane inflammatory changes of the gallbladder and the features of hormonal expression in the development of dysplasia-carcinoma consequence
Downloads
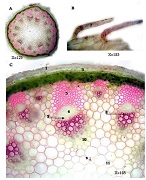
Gallbladder carcinoma is the most common tumour of the biliary tract. It is relatively rare in Western countries. However, it is widespread in different regions of the world, especially in developing countries. The most effective treatment method for gallbladder carcinoma is radical cholecystectomy. However, unfortunately, only 10-30% of patients are subject to this treatment method, since 70-90% of cases are diagnosed at an advanced stage. The development of gallbladder carcinoma is associated with various environmental and genetic factors, also the presence of chronic inflammation and/or exposure to specific chemicals, heavy metals, and nutritional factors. The exact mechanism of how gallbladder carcinoma develops in the background of cholelithiasis is still not completely clear. During inflammatory lesions of the gallbladder, changes in the proliferation index of the gallbladder epithelium have not been studied yet. In addition to proliferative markers, it has also been shown that the reduction of cell apoptotic activity plays an important role in the pathogenesis of many tumours. However, literature data on the apoptotic activity of gallbladder carcinomas are incomplete and contradictory.
Downloads
R. L. Siegel and K. D. Miller, “Cancer Statistics , 2020,” vol. 70, pp. 7–30, 2020.
F. Graur, E. Mois, S. Margarit, C. Hagiu, and al Hajjar, “Gallbladder carcinoma. Surgical management of gallblad-der carcinoma. An analysis of 37 cases,” vol. 89, pp. 501–506.
S. E. Lee et al, “Practical guidelines for the surgical treatment of gallbladder cancer.,” J. Korean Med. Sci, vol. 29, pp. 1333–1340, Oct. 2014.
v. Ostwal et al, “Treatment of advanced Gall bladder cancer in the real world-can continuation chemotherapy improve outcomes?,” J. Gastrointest. Oncol, vol. 8, pp. 368–376, Apr. 2017.
v. Dilalla, G. Chaput, T. Williams, and K. Sultanem, “Radiotherapy side effects: integrating a survivorship clinical lens to better serve patients.,” Curr. Oncol., vol. 27, pp. 107–112, Apr. 2020.
K. Nurgali, R. T. Jagoe, and R. Abalo, “Editorial: Adverse Effects of Cancer Chemotherapy: Anything New to Improve Tolerance and Reduce Sequelae?,” Front Pharmacol, vol. 9, p. 245, 2018.
A. Sharma, K. L. Sharma, A. Gupta, A. Yadav, and A.Kumar, “Gallbladder cancer epidemiology, pathogenesis and molecular genetics: Recent update.,” World J. Gastroenterol, vol. 23, pp. 3978–3998, 2017.
S. Ryu, Y. Chang, K. E. Yun, H.-S. Jung, J. H. Shin, and H. Shin, “Gallstones and the Risk of Gallbladder Cancer Mortality: A Cohort Study.,” Am. J. Gastroenterol., vol. 111, pp. 1476–1487, Oct. 2016.
J. A. Espinoza et al., “The inflammatory inception of gallbladder cancer.,” Biochim. Biophys. Acta, vol. 1865, pp. 245–254, Apr. 2016.
C. H. C. Pilgrim, R. T. Groeschl, K. K. Christians, and T. C. Gamblin, “Modern perspectives on factors predisposing to the development of gallbladder cancer.,” HPB (Oxford)., vol. 15, pp. 839–844, Nov. 2013.
R. Hundal and E. A. Shaffer, “Gallbladder cancer: epidemiology and outcome.,” Clin. Epidemiol., vol. 6, pp. 99–109, 2014.
J. H. Kim et al., “Programmed death-ligand 1 expression and its correlation with clinicopathological parameters in gallbladder cancer,” J Pathol Transl Med, vol. 54, no. 2, pp. 154–164, 2020, doi: 10.4132/jptm.2019.11.13.
S. K. Mathur et al., “Correlation of gallstone characteristics with mucosal changes in gall bladder.,” Trop. Gastroenterol., vol. 33, pp. 39–44, 2012.
N. Katabi, “Neoplasia of Gallbladder and Biliary Epithelium.”
Y. Xue, B. Quigley, G. Akkas, and V. Adsay, “Neoplastic precursors (dysplasia, intraepithelial neoplasia) of the gallbladder and biliary tract: Terminology, classification, pathologic diagnosis, and clinical significance,” Diagnostic Histopathology, vol. 21, no. 8. Elsevier Ltd, pp. 323–331, Aug. 01, 2015. doi: 10.1016/j.mpdhp.2015.06.023.
I. Roa, X. de Aretxabala, J. C. Araya, and J. Roa, “Preneoplastic lesions in gallbladder cancer,” in Journal of Surgical Oncology, Jun. 2006, vol. 93, no. 8, pp. 615–623. doi: 10.1002/jso.20527.
A. L. A. Meirelles-Costa, C. J. C. Bresciani, R. O. Perez, B. H. Bresciani, S. A. C. Siqueira, and I. Cecconello, “Are histological alterations observed in the gallbladder precancerous lesions?,” Clinics, vol. 65, no. 2, pp. 143–150, 2010, doi: 10.1590/S1807-59322010000200005.
R. Dixit, V. K. Shukla, and M. Pandey, “World Journal of Pathology Molecular alterations in gallbladder cancer,” 2012. [Online]. Available: www.npplweb.com/wjp/fulltext/1/7
H. Nakamura et al., “Genomic spectra of biliary tract cancer.,” Nat. Genet., vol. 127, pp. 175–186, Jun. 2015.
M. Teh, A. Wee, M. R. C. Path, and G. C. Raju, “An lmmunohistochemical Study of p53 Protein in Gallbladder and Extrahepatic Bile Duct/Ampullary Carcinomas.”
M. Ghosh, P. Sakhuja, S. Singh, and A. Agarwal, “P53 and beta-catenin expression in gallbladder tissues and correlation with tumor progression in gallbladder cancer,” Saudi Journal of Gastroenterology, vol. 19, no. 1, pp. 34–39, Jan. 2013, doi: 10.4103/1319-3767.105922.
X. Sun and P. D. Kaufman, “Ki-67: more than a proliferation marker,” Chromosoma, vol. 127, Jun. 2018.
S. Halder, S. Kundu, J. Chakraborty, and S. Chakrabarti, “Significance of HER2 and Ki-67 in Preneoplastic Lesions and Carcinoma of Gallbladder.,” vol. 50, pp. 848–854, Dec. 2019.
Y. Shen et al., “Liensinine induces gallbladder cancer apoptosis and G2/M arrest by inhibiting ZFX-induced PI3K/AKT pathway.,” Acta Biochim. , vol. 51, pp. 607–614, Jun. 2019.
S. K. Mondal, D. Bhattacharjee, P. K. Mandal, and S. Biswas, “Histopathological study of gallbladder carcinoma and its mimics with role of carcinoembryonic antigen immunomarker in resolving diagnostic difficulties,” Indian Journal of Medical and Paediatric Oncology, vol. 38, no. 4, pp. 411–415, Oct. 2017, doi: 10.4103/ijmpo.ijmpo_230_15.
Y.-L. Choi et al., “An Immunohistochemical Study of the Expression of Adhesion Molecules in Gallbladder Lesions,” 2004. [Online]. Available: http://www.jhc.org
R. Saranga Bharathi et al., “Female sex hormone receptors in gallbladder cancer.,” vol. 46, pp. 143–148, Jun. 2015.
Sunwang Xu, Ming Zhan, and Jian Wang, “Epithelial-to-mesenchymal transition in gallbladder cancer: from clinical evidence to cellular regulatory networks,” Nov. 2017.
A. Dongre and R. A. Weinberg, “New insights into the mechanisms of epithelial–mesenchymal transition and implications for cancer,” Nat. Rev. Mol. Cell Biol, vol. 20, pp. 69–84, 2019.
R. Kalluri and R. A. Weinberg, “The basics of epithelial-mesenchymal transition,” Journal of Clinical Investigation, vol. 119, no. 6. pp. 1420–1428, Jun. 01, 2009. doi: 10.1172/JCI39104.
C. Bizama et al., “Targeting specific molecular pathways holds promise for advanced gallbladder cancer therapy,” Cancer Treatment Reviews, vol. 41, no. 3. W.B. Saunders Ltd, pp. 222–234, Mar. 01, 2015. doi: 10.1016/j.ctrv.2015.01.003.
X. Song, Y. Hu, Y. Li, R. Shao, F. Liu, and Y. Liu, “Overview of current targeted therapy in gallbladder cancer,” Signal Transduction and Targeted Therapy, vol. 5, no. 1. Springer Nature, Dec. 01, 2020. doi: 10.1038/s41392-020-00324-2.

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.