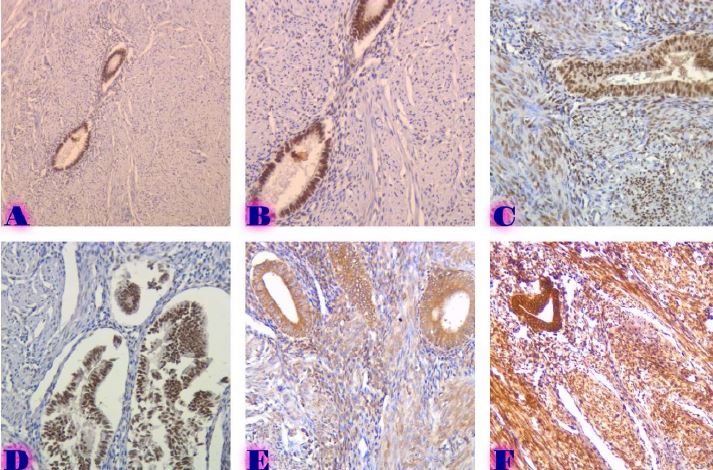
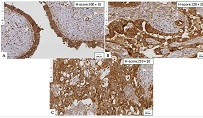
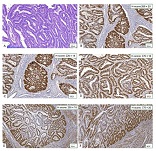
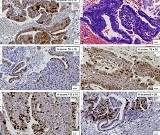
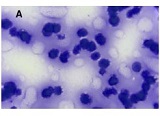
Features of distribution of intratumoral lymphocytes in ovarian epithelial tumours of different histological types and degree of malignancy
Downloads
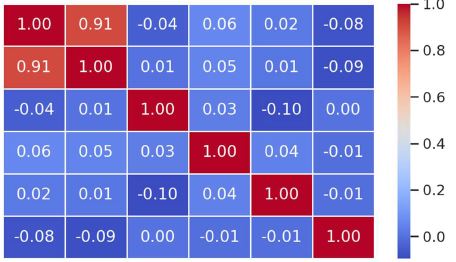
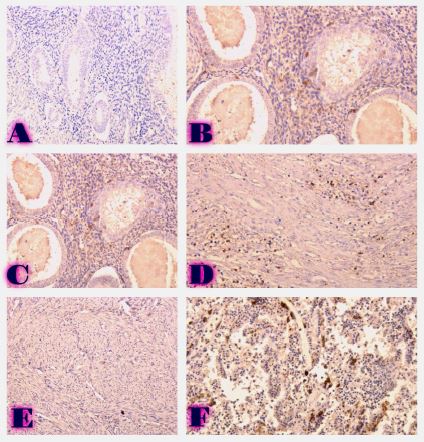
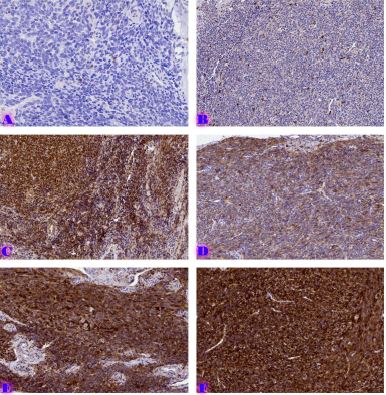
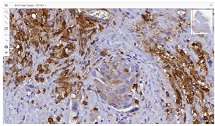
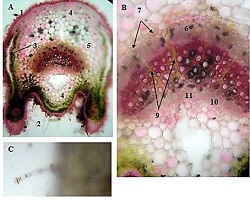
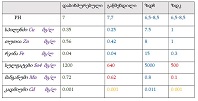
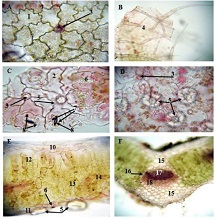
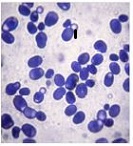
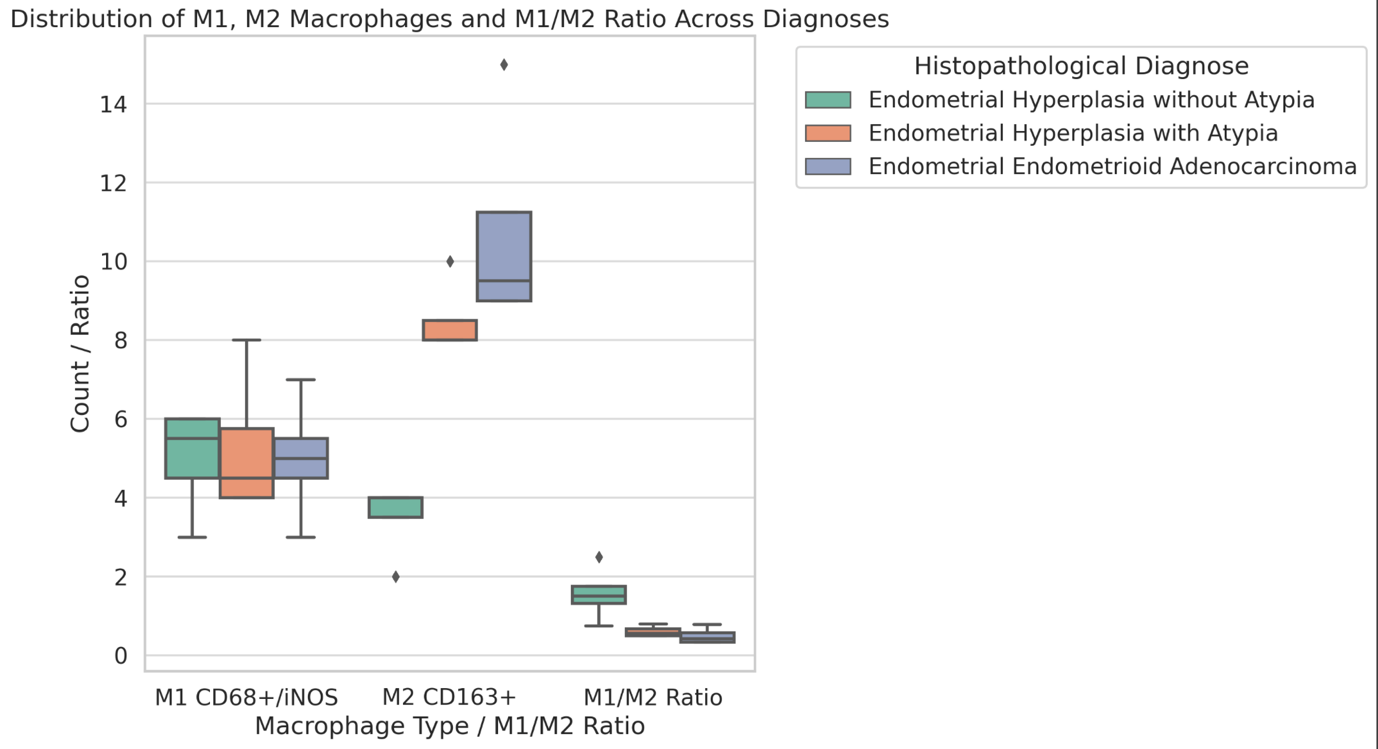
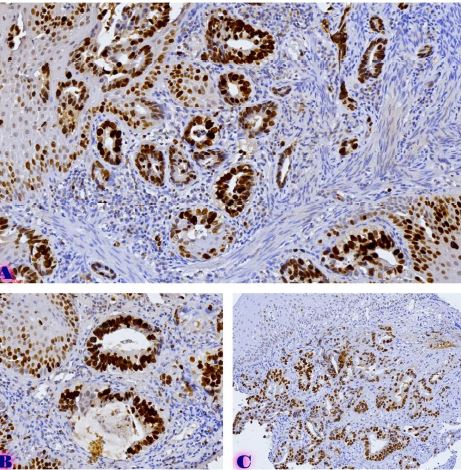
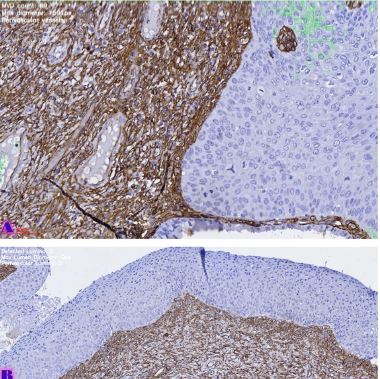
Ovarian cancer is the leading cause of death from gynaecological cancers worldwide. In Georgia, ovarian cancer ranks fourth in terms of prevalence, and third in terms of mortality rate. According to the latest epidemiological data, there will be 21,421 new cases of ovarian cancer and 13,770 deaths from ovarian cancer in the United States in 2021. Due to the lack of early screening methods and asymptomatic clinical courses, most ovarian cancer is diagnosed at an advanced stage, when the prognosis of the disease is already poor. Despite the advances in modern medical treatment and surgery, ovarian carcinoma remains the most lethal gynaecological cancer. The 5-year survival rate is 46% for all stages combined. The microenvironment of ovarian carcinomas is mainly represented by macrophages, dendritic cells, neutrophils and lymphocytes. Epithelial ovarian carcinoma-infiltrating lymphocytes (TIL) have attracted much interest in the last five years. Ovarian cancer is a heterogeneous disease concerning tumour-infiltrating lymphocytes and TILs. In terms of histological subtypes, most studies include only high-grade serous carcinomas of the ovary, and studies on other histological types are scarce. The results of our study show that the quantitative evaluation of T lymphocytes and their subpopulations does not show a statistically reliable correlation between different histological types of tumours, which may be due to the intratumoral heterogeneity and individual specificity of tumours.
Downloads
D. L. Longo and R. C. Young, “The natural history and treatment of ovarian cancer,” Annu Rev Med, vol. 32, pp. 475–490, 1981, doi: 10.1146/annurev.me.32.020181.002355.
J. Ferlay et al., “Estimating the global cancer incidence and mortality in 2018: GLOBOCAN sources and methods,” Int J Cancer, vol. 144, no. 8, pp. 1941–1953, Apr. 2019, doi: 10.1002/ijc.31937.
P. Achimas-Cadariu, P. Kubelac, A. Irimie, I. Berindan-Neagoe, and F. Rühli, “Evolutionary perspectives, heterogeneity and ovarian cancer: a complicated tale from past to present,” J Ovarian Res, vol. 15, no. 1, pp. 1–13, Dec. 2022, doi: 10.1186/S13048-022-01004-1/FIGURES/1.
M. Timmermans, G. S. Sonke, K. K. van de Vijver, M. A. van der Aa, and R. F. P. M. Kruitwagen, “No improvement in long-term survival for epithelial ovarian cancer patients: A population-based study between 1989 and 2014 in the Netherlands,” Eur J Cancer, vol. 88, pp. 31–37, Jan. 2018, doi: 10.1016/j.ejca.2017.10.030.
M. C. A. Wouters et al., “Treatment regimen, surgical outcome, and t-cell differentiation influence prognostic benefit of tumor-infiltrating lymphocytes in high-grade serous ovarian cancer,” Clinical Cancer Research, vol. 22, no. 3, pp. 714–724, Feb. 2016, doi: 10.1158/1078-0432.CCR-15-1617.
S. Zhan et al., “New Insights into Ferroptosis Initiating Therapies (FIT) by Targeting the Rewired Lipid Metabolism in Ovarian Cancer Peritoneal Metastases.,” Int J Mol Sci, vol. 23, no. 23, Dec. 2022, doi: 10.3390/ijms232315263.
Y. Xu, F. Zuo, H. Wang, J. Jing, and X. He, “The current landscape of predictive and prognostic biomarkers for immune checkpoint blockade in ovarian cancer.,” Front Immunol, vol. 13, p. 1045957, Oct. 2022, doi: 10.3389/fimmu.2022.1045957.
S. Gomez et al., “Inhibiting DNA methylation and RNA editing upregulates immunogenic RNA to transform the tumor microenvironment and prolong survival in ovarian cancer,” J Immunother Cancer, vol. 10, no. 11, p. e004974, Nov. 2022, doi: 10.1136/jitc-2022-004974.
J. M. Santos et al., “Oncolytic adenovirus shapes the ovarian tumor microenvironment for potent tumor-infiltrating lymphocyte tumor reactivity,” J Immunother Cancer, vol. 8, no. 1, Jan. 2020, doi: 10.1136/jitc-2019-000188.
Y. R. Chung, H. J. Kim, M. H. Jang, and S. Y. Park, “Prognostic value of tumor infiltrating lymphocyte subsets in breast cancer depends on hormone receptor status,” Breast Cancer Res Treat, vol. 161, no. 3, pp. 409–420, Feb. 2017, doi: 10.1007/s10549-016-4072-9.
G. Mittica et al., “Adoptive immunotherapy against ovarian cancer,” J Ovarian Res, vol. 9, no. 1, May 2016, doi: 10.1186/s13048-016-0236-9.
S. E. Stanton and M. L. Disis, “Clinical significance of tumor-infiltrating lymphocytes in breast cancer,” J Immunother Cancer, vol. 4, no. 1, Oct. 2016, doi: 10.1186/s40425-016-0165-6.
P. P. Santoiemma and D. J. Powell, “Tumor infiltrating lymphocytes in ovarian cancer,” Cancer Biol Ther, vol. 16, no. 6, pp. 807–820, Jan. 2015, doi: 10.1080/15384047.2015.1040960.
Copyright (c) 2022 Rusudan Devadze, Arsen Gvenetadze, George Burkadze, Shota Kepuladze

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.