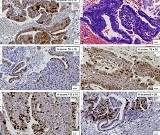
Clinical and Immunological Study of the Effectiveness of the Medications, Lazolex and Zovirax, during the Complex Treatment of Chronic Recurrent Herpetic Stomatitis
Downloads
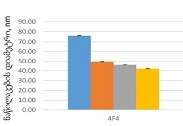
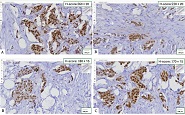
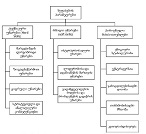
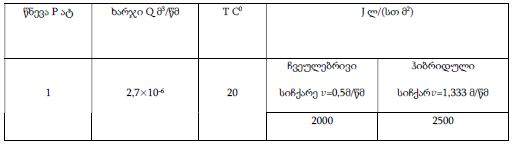
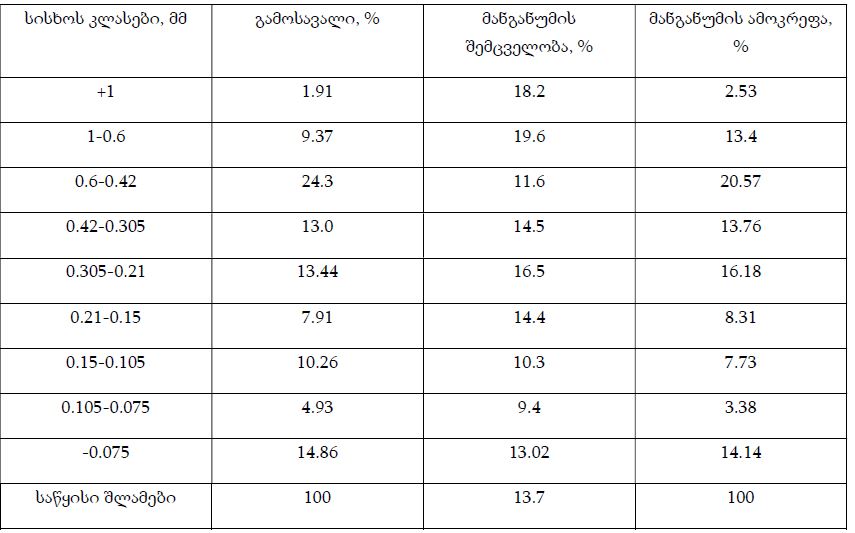
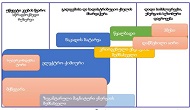
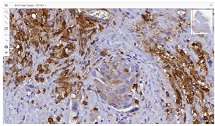
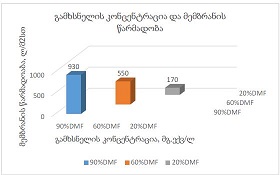
At present, our country continues intensive research to find and introduce into practice new natural medicinal preparations made from ecologically pure endemic plants of Georgia. An example of such an agent in the Iveria-Pharma company is a Georgian medication - LAZOLEX (extract of the pericarpium of an unripe walnut), which has passed the necessary preclinical tests and now is used as an antiherpetic agent. We found positive immunotropic effects of Lazolex on healthy volunteers. Therefore, we considered it necessary to study the antiviral effects of the drug and its immunomodulatory properties in a clinical setting, specifically its effect on chronic herpetic stomatitis. First of all, it was shown that the immune system status of the patients was in an apparent correlation with the severity of the course of herpes stomatitis, i.e. the most severe immunosuppression was recorded in patients with severe stomatitis. It should be noted that this medication not only doubles the efficiency of the results of antiviral treatment but also serves as an immune restoration agent in patients with herpetic stomatitis. As a result of a parallel study of Zovirax and Lazolex, a high clinical activity of both drugs was recorded. However, the presence of pronounced immunocorrective properties of Lazolex manifested itself in an improvement of the quality of patient treatment: active tissue regeneration and a significant decrease in the timing of exacerbation of local herpetic lesions, an increase in the duration of remission. Conducted clinical, laboratory, and immunological studies allow us to recommend Lazolex for active use in dental practice for viral diseases.
Downloads
N. Abashidze – “Microbiological and immunomorphological aspects of differential diagnosis and treatment of the diseases of the oral mucosa” - Dissertation, 2005
M. Gogotishvili, N. Abashidze, M. Iverieli, Kh. Gogishvili, N. Gogebashvili - ” Use of Lazolex in the complex treatment of chronic recurrent herpetic stomatitis” - Collection of Scientific Works of TSMU, 2014; XLVIII: 51-55
M. Gogotishvili, N. Abashidze, M. Iverieli, Kh. Gogishvili, N. Gogebashvili - ”Use of Lazolex in the complex treatment of chronic recurrent herpetic stomatitis” TSMU Collection of Scientific Works, 2015; XLIX: 32-35
Nino Korsantia, Nato Korsantia, B. Korsantia - “Prospects for the use of Plaferon-containing adhesive plates in inflammatory diseases of the oral cavity” experim. Clinic. Journal of Medicine., 2020: #4, 88-92
N. Alavidze, M. Gogotishvili - et al. “Study of the Antiherpetic Properties of Lazolex in Various Experimental Models” J. Expert. Clinical Medicine 2013; 5: 48-53
V.A. Isakov, D.V. Isakov – “Immunomodulators in the Treatment and Prevention of Herpesvirus Infections” Clinical Honey. 2015; 4: 46-51
Nino Korsantia, A. Katsitadze, Nato Korsantia, B. Korsantia – “Clinical and Immunotropic Effectiveness of Licopid During Oral Herpes” J. Experiment. Clinical Medicine 2017; 5: 81-84
D.K. Novikov – “Handbook of clinical immunology and allergology” Minsk, "Belarus", 1987; 223s.
V.D. Solovyov, T.A. Bektimirov – “Interferons in the Theory and Practice of Medicine” M., "Medicine", 1981, 400 p.
www.iveriapharma.com/index.php/products/lazolex
S.A. Al-Maweri, B. Kalakonda, N.A. AlAizari – “Efficacy of low-level laser therapy in the management of recurrent herpes labialis: a systematic review” Lasers in Medical Science 2018; 33(7); 1423-1430.
J. Amir - et al. “Treatment of herpes simplex gingivostomatitis with aciclovir in children: a randomized double-blind placebo-controlled study” BMJ 1997; 314(7097): 1800-1803.
M. Boeckh, L. Corey – “Adoptive immunotherapy of viral infections: should infectious disease embrace cellular immunotherapy?” J. Infect. Dis. 2017; 216 (8): 926-928.
J. Сummins - et al. “Oral therapy with human interferon” Arch. Imm. Ther. Exp., 1993; 41, 193-197.
S.B. Carter, E.J. Cohen – “Development of herpes simplex virus infectious epithelial keratitis during oral acyclovir therapy and response to topical antivirals” - Cornea, 2016, 85-120.
R. Du, L. Wang - et al. “A novel glycoprotein D-specific monoclonal antibody neutralizes herpes simplex virus” Antiviral. Res., 2017; 147: 131-141.
J. Epstein - et al. “Complex management of resistant oral herpes simplex virus infection following hematopoietic stem cell transplantation: potential role of topical cidofovir” // Support Care Cance, 2016; 24(8): 3603-3606.
[Guideline] Centers for Disease Control and Prevention 2015 – “Sexually Transmitted Diseases Treatment Guidelines” https://www.cdc.gov/std/tg2015/default.htm. 2017; January 25, Accessed: December 5, 2017.
M.K. Kamalova–“ Use of laser therapy in the treatment of chronic recurrent herpetic stomatitis for children” Eur. Sci. Rev. 2018; 7-8; 120-121.
McDonald J.H. Handbook of Biological Statistics, 3rd ed. Baltimore, Sparkly House Publishing. 2014.
C. Laggis, D. Wada, A. Shah, J. Zussman – “Eosinophils are surprisingly common in biopsy specimens of cutaneous herpes simplex virus and varicella zoster virus infections: Results of a comprehensive histopathologic and clinical appraisal” J. Cutan. Pathol., 2020; 47(1): 6-11.
I. Ptaszyńska-Sarosiek, J. Dunaj, A. Zajkowska – “Post-mortem detection of six human herpesviruses (HSV-1, HSV-2, VZV, EBV, CMV, HHV-6) in trigeminal and facial nerve ganglia by PCR” Peer. J. 2019; 6: e6095.
S. Mackenzie-Dyck, L. Latimer, E. Atanley, J. Kovacs-Nolan, S. Attah-Poku, LA. Babiuk, van Drunen Littel- S. van den Hurk – “Immunogenicity of a bovine herpesvirus 1 glycoprotein D DNA vaccine complexed with bovine neutrophil beta-defensin 3” -Clin Vaccine Immunol. 2015, 79–90.
J. Peer – “Herpesviruses (HSV-1, HSV-2, VZV, EBV, CMV, HHV-6) in trigeminal and facial nerve ganglia” by PCR. 2019; 6: e6095.
A. Subramaniam, W. Britt – “Herpesviridae Infection: Prevention, Screening, and Management” Clin. Obstet. Gynecol. 2018; 61(1): 157-176.
E. Jouanguy, V. Béziat, TH. Mogensen, JL. Casanova, SG. Tangye, SY. Zhang – “Human inborn errors of immunity to herpes viruses” - Curr Opin Immunol. 2020, 104-190.
Copyright (c) 2023 GEORGIAN SCIENTISTS

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.