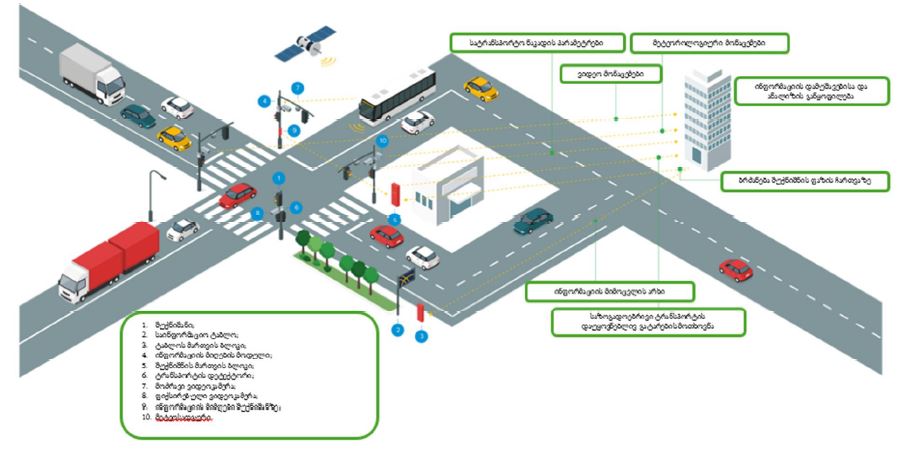
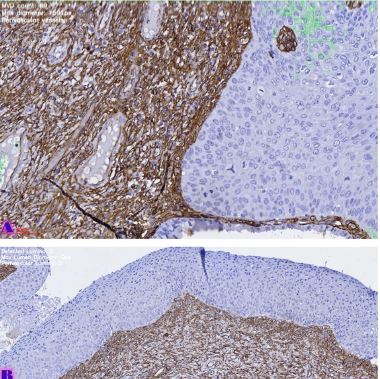
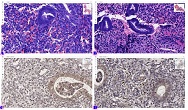
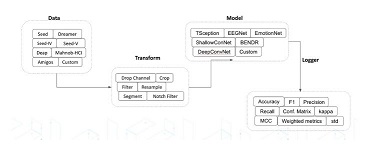
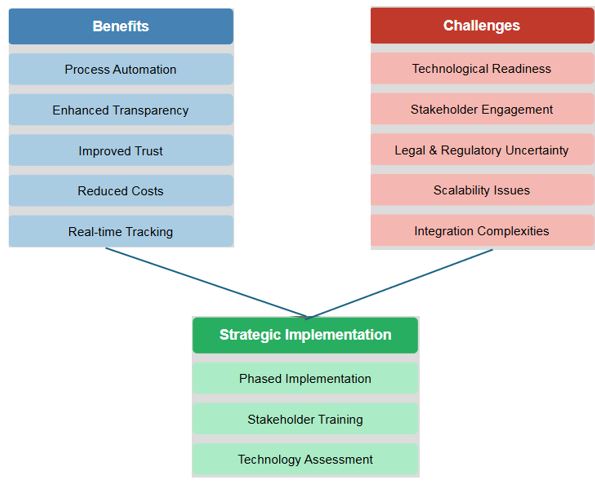
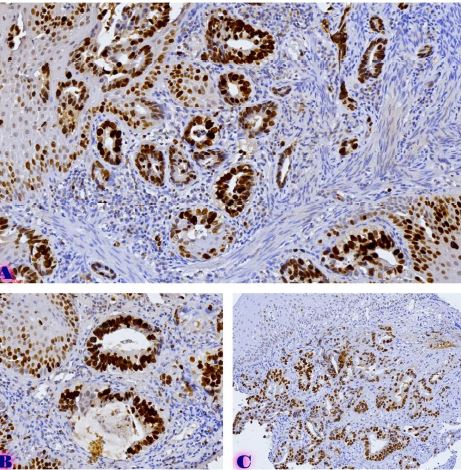
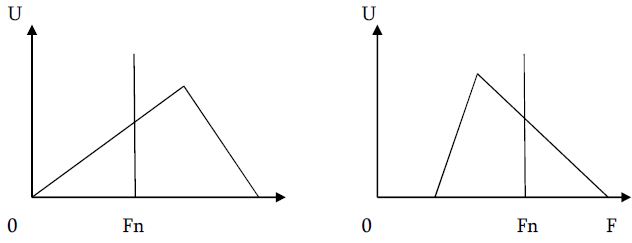
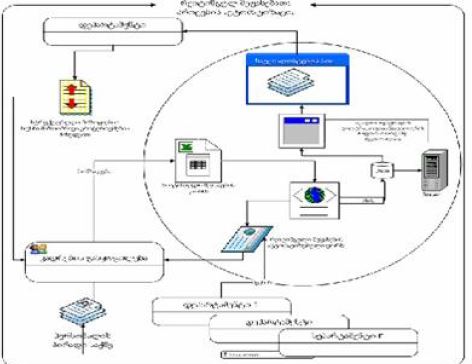
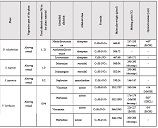
Thermal pain perception during different satiety levels in males and females across follicular and luteal phases of the ovarian-menstrual cycle
Downloads
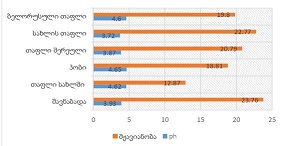
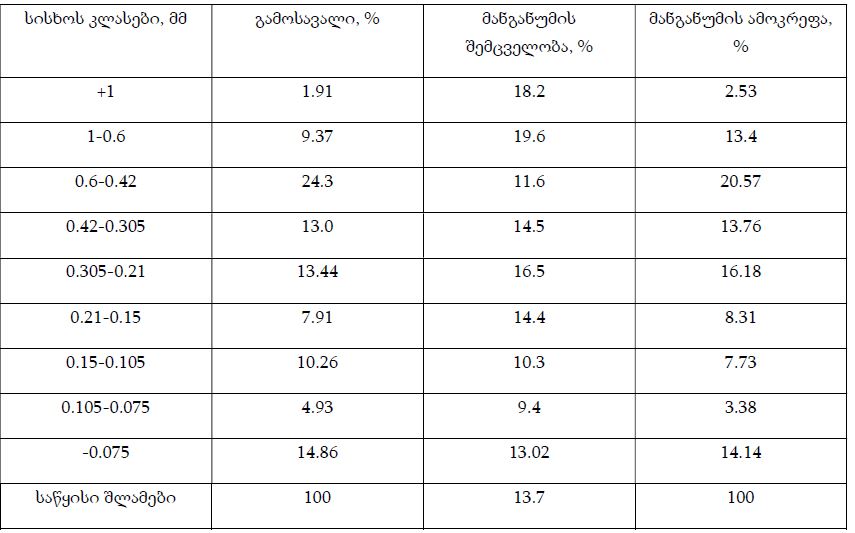
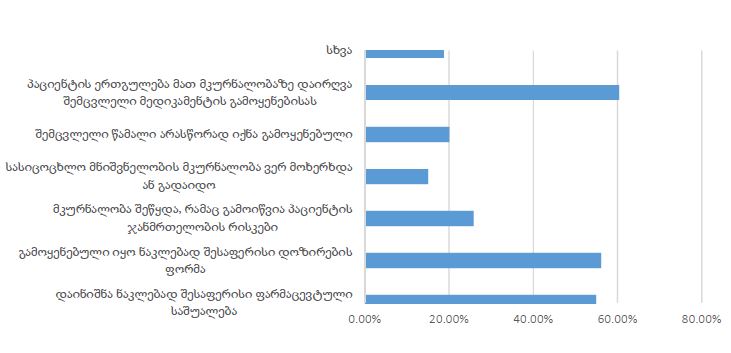
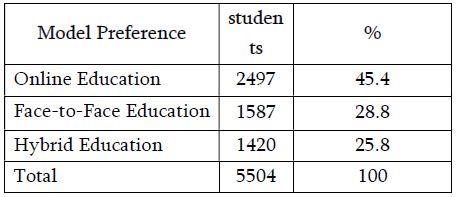
Nowadays it is known that sex hormones play an important role not only in the reproductive system but also in thermoregulation, somatosensory control, and pain perception. Several studies have shown that women are less tolerant of pain and have higher sensitivity and predisposition to somatization and pain chronification. In addition to sex, feeding status is also an essential factor for pain perception. Metabolic factors and glucose levels may play a role in the sensation of pain. In this paper, we report an evaluation of thermal pain thresholds induced by heat and cold stimulation in males and females during primary (pre-resorption) and secondary (metabolic) satiety. The obtained data showed that in both sensory-motor satiety and metabolic satiety, the heat pain threshold was significantly higher in males than in females in the follicular and luteal phases of the ovarian-menstrual cycle. Further studies are needed to detect more details on the influence of food satiety levels on pain perception regarding sex differences.
Downloads
Treede RD. The International Association for the Study of Pain definition of pain: as valid in 2018 as in 1979, but in need of regularly updated footnotes. Pain Rep. 2018;3(2): e643. doi: 10.1097/PR9. 0000000000000643.
Kvachadze I, Tsagareli MG, Dumbadze Z. An overview of ethnic and gender differences in pain sensation. Georgian Med News. 2015;(238):102-108.
Thurston KL, Zhang SJ, Wilbanks BA, Billings R, Aroke EN. A systematic review of race, sex, and socioeconomic status differences in postoperative pain and pain management. J Perianesth Nurs. 2022; S1089-9472(22)00516-0. doi: 10.1016/j.jopan.2022.09.004.
Ruschak I, Montesó-Curto P, Rosselló L, Aguilar Martín C, Sánchez-Montesó L, Toussaint L. Fibromyalgia syndrome pain in men and women: A scoping review. Healthcare (Basel) 2023; 11(2): 223. doi: 10.3390/healthcare11020223.
van Kessel L, Teunissen D, Lagro-Janssen T. Sex-gender differences in the effectiveness of treatment of irritable bowel syndrome: A systematic review. Int J Gen Med. 2021;14:867-884. doi: 10.2147/IJGM.S291964.
Maranini B, Bortoluzzi A, Silvagni E, Govoni M. Focus on sex and gender: What we need to know in the management of rheumatoid arthritis. J Pers Med. 2022;12(3):499. doi: 10.3390/jpm12030499.
Racine M, Sole E, Sanchez-Rodriguez E, Tome-Pires C, Roy R, Jensen MP, Miro J, Moulin DE, Cane D. An evaluation of sex differences in patients with chronic pain undergoing an interdisciplinary pain treatment program. Pain Practice. 2020;20(1):62-74. doi:10.1111/papr.12827
Fillingim RB, King CD, Ribeiro-Dasilva MC, Rahim-Williams B, Riley JL. Sex, gender, and pain: a review of recent clinical and experimental findings. J Pain. 2009;10(5):447-485. doi: 10.1016/j. jpain.2008.12.001.
Sorge RE, Totsch SK. Sex differences in pain. J Neurosci Res. 2017;95(6):1271-1281. doi: 10.1002/ jnr.23841.
Herren RY. The effect of high and low female sex hormone concentration on the two-point threshold of pain and touch and upon tactile sensitivity. J Exp Psychol. 1933;16(2):324–327.
Boerner KE, Chambers CT, Gahagan J, Keogh E, Fillingim RB, Mogil JS. Conceptual complexity of gender and its relevance to pain. Pain. 2018; 159(11):2137-2141. doi: 10.1097/j.pain. 0000000000001275
Fillingim RB, King CD, Ribeiro-Dasilva MC, Rahim-Williams B, Riley JL. Sex, gender, and pain: a review of recent clinical and experimental findings. J Pain. 2009;10(5):447-485. doi: 10.1016/j. jpain.2008.12.001.
Niesters M, Dahan A, Kest B, Zacny J, Stijnen T, Aarts L, Sarton E. Do sex differences exist in opioid analgesia? A systematic review and meta-analysis of human experimental and clinical studies. Pain. 2010;151(1):61-68. doi: 10.1016/j.pain.2010.06.012.
Amandusson A, Blomqvist A. Estrogenic influences in pain processing. Front Neuroendocrinol. 2013;34(4):329-349. doi: 10.1016/j.yfrne.2013.06.001.
Stening KD, Berg G, Hammar M, Voster H, Eriksson O, Amandusson A, Blomqvist A. Influence of estrogen levels on thermal perception, pain thresholds, and pain tolerance: studies on women undergoing in vitro fertilization. J Pain. 2012;13(5):459-466. doi: 10.1016/j.jpain.2012.01.446.
Piroli A, Mattei A, Carta G, D'Alfonso A, Palermo P, Marinangeli F. et al. Influence of the menstrual cycle phase on pain perception and analgesic requirements in young women undergoing gynecological laparoscopy. Pain Practice. 2019;19(2):140-148. doi: 10.1111/papr.12727.
Smith YR, Stohler CS, Nichols TE, Bueller JA, Koeppe RA, Zubieta JK. Pronociceptive and antinociceptive effects of estradiol through endogenous opioid neurotransmission in women. J Neurosci. 2006;26(21):5777-5785. doi: 10.1523/JNEUROSCI.5223-05.2006.
Anjana Y, Reetu K. Effect of food intake on pain perception in healthy human subjects. J Evol Med Dental Sci. 2014;3(29):7984-7988. doi: 10.14260/jemds/2014/3000
Amandusson Å, Blomqvist A. Estrogenic influences in pain processing. Front Neuroendocrinol. 2013;34(4):329-349. doi: 10.1016/j.yfrne.2013.06.001.
Mercer ME, Holder MD. Antinociceptive effects of palatable sweet ingesta on human responsivity to pressure pain. Physiol Behav. 1997;61(2):311-318. doi: 10.1016/s0031-9384(96)00400-3.
Lee JH, McCarty R. Glycemic control of pain threshold in diabetic and control rats. Physiol Behav. 1990;47(2):225-230. doi: 10.1016/0031-9384(90)90135-q.
Pilozzi A, Carro C, Huang X. Roles of β-endorphin in stress, behavior, neuroinflammation, and brain energy metabolism. Int J Mol Sci. 2020;22(1):338. doi: 10.3390/ijms22010338.
Malagelada JR, Go VL, Summerskill WH. Different gastric, pancreatic, and biliary responses to solid-liquid or homogenized meals. Dig Dis Sci. 1979;24(2):101-110. doi: 10.1007/BF01324736.
Moore JG, Schenkenberg T. Psychic control of gastric acid: Response to anticipated feeding and biofeedback training in man. Gastroenterology. 1974;66(5):954-959.
Apkhazava M, Kvachadze I, Tsagareli M, Mzhavanadze D, Chakhnashvili M. Sex differences in response to experimentally induced pain. Georgian Med News. 2019; #2(286):119-124.
Gvasalia T, Kvachadze I, Giorgobiani T. Sensitivity to mechanical pain based on satiety levels in women. Georgian Med News. 2021; #1(310):83-86.
Castellote JM, Valls-Solé J. Temporal relationship between perceptual and physiological events triggered by nociceptive heat stimuli. Sci Rep. 2019;9(1):3264. doi: 10.1038/s41598-019-39509-3.
Klatzkin RR, Mechlin B, Girdler SS. Menstrual cycle phase does not influence gender differences in experimental pain sensitivity. Eur J Pain. 2010;14(1):77-82. doi: 10.1016/j.ejpain.2009.01.002.
Kumar P, Jaspreet K, Pujara J, Anand JS. Correlation of serum oestrogen level with duration of post-operative analgesia. Indian J Anaesthesia. 2007;51(6):519-524.
Copyright (c) 2023 GEORGIAN SCIENTISTS

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.